These environmental changes create a phenomenon known as the “first night effect”, which implicates changes in sleep quality and efficiency resulting in inaccurate and unrepresentative results. Polysomnographic studies are typically conducted in a sleep laboratory which is an unfamiliar environment for patients and is associated with the discomfort of being connected to a recording device with several wires. The in-laboratory PSG has several challenges including significant financial, human, and healthcare costs. In addition, a nasal pressure transducer is used for snoring detection. Typically, oxygen saturation is measured using a pulse oximeter attached to the patient’s finger. For monitoring of respiratory effort, dual thoracoabdominal belts are used. For identification of obstructive events, an oronasal airflow sensor is used to monitor the airflow. The overnight in-laboratory PSG involves the concurrent recording of physiologic signals during sleep, including the electroencephalogram (EEG), electrooculogram (EOG), electromyogram (EMG), and electrocardiogram (ECG). These may include excessive daytime sleepiness, hypertension, and depression. For some, the presence of the clinical sequelae of apnea is considered when evaluating the clinical severity of OSA. Other measures of the disease activity include the degree of hypoxemia and the arousal index. OSA is considered mild with an AHI between 5 and 15/hour moderate with an AHI of 15 and 30/hour and severe with an AHI ≥ 30/hour. The severity of OSA is classified according to the apnea-hypopnea-index (AHI), which is the number of obstructive events per hour of sleep. The gold-standard method for the diagnosis of OSA is an overnight in-laboratory polysomnography (PSG). The diagnosis and treatment of OSA may decrease the recurrence and/or severity of cardiac arrhythmia.

OSA has been identified as a risk factor for the induction and progression of significant cardiac rhythm disturbance including atrial fibrillation.

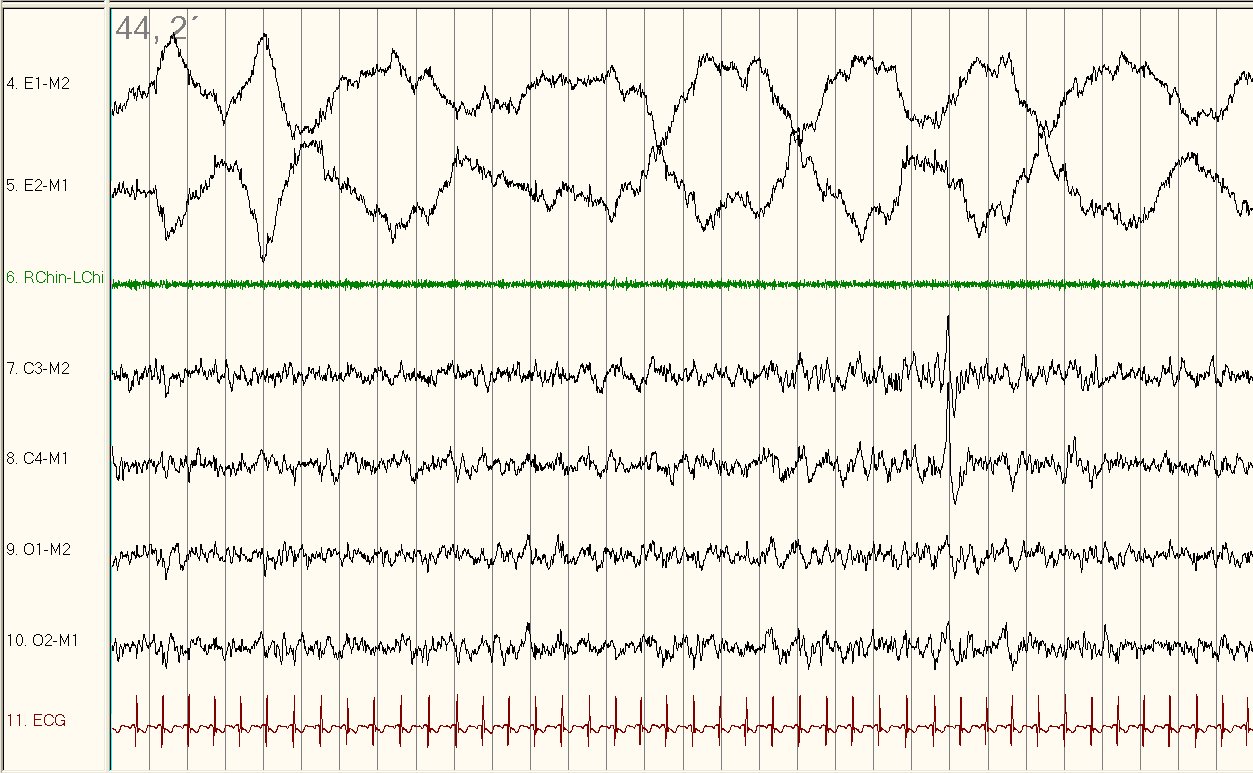
Obstructive sleep apnea (OSA) is a common disorder associated with significant cardiovascular morbidities. Ambulatory studies incorporating EEG may provide a reliable, convenient, and economically efficient method for sleep assessment and there appears to be no significant night-to-night variability. There is no significant difference in the respiratory parameters obtained during two consecutive nights of ambulatory sleep testing. There were no other significant differences in the sleep architecture, respiratory indices, and other sleep parameters between the first and the second night of the ambulatory sleep recording. REM latency was shorter during the second night of sleep recording ( ). The two nights of the ambulatory sleep testing showed consistent results with an excellent test-retest reliability for the AHI (ICC = 0.813). In patients with OSA, the sleep efficiency and the percentage of slow wave sleep were reduced however, the arousal and periodic limb movement indices were increased compared to patients without OSA. In the total sample, the sleep efficiency was reduced, and sleep onset latency was longer compared to a reference population of the same age. OSA (AHI ≥ 5/h) was detected in 85% of patients. Patients underwent two consecutive nights of self-applied in-home sleep testing replete with electroencephalogram (EEG) recording. Consecutive patients with unknown OSA status were recruited from arrhythmia clinics. We aimed to (1) determine the sleep architecture in arrhythmia patients (2) detect differences in sleep parameters between patients with and without OSA and (3) compare the results of two consecutive nights of unattended ambulatory sleep testing.

Ambulatory sleep testing may provide an alternative method for detection of OSA under realistic conditions compared to in-laboratory polysomnography. Obstructive sleep apnea (OSA) is common and usually underdetected in patients with cardiac arrhythmia.
